The UCSF Community Living Policy Center and the Institute for Health and Aging partnered to conduct an evaluation of Cal MediConnect (CMC). One goal of this evaluation was to assess beneficiaries' experiences with care, include access, quality, and coordination over time. To that end, researchers conducted a longitudinal telephone survey with three groups of dually eligible beneficiaries: those enrolled in CMC, those who opted out, and those in non-demonstration (non-CCI) counties. Key findings from the first telephone survey (T1) were reported in 2016.
Reports & Publications

This document provides guidance on how States can, in the process of implementing the new federal regulations outlining new procedural requirements for managed care plans' grievance and appeal systems, ensure that people with disabilities have equal access to the grievance and appeal and State fair hearing systems, as mandated by Section 504 of the Rehabilitation Act ("Rehab Act"), the Americans with Disabilities Act ("ADA"), and Section 1557 of the Affordable Care Act ("ACA").
Researchers at the University of California conducted an evaluation of the implementation and impact of the CMC program on health systems and beneficiaries. This research brief examines the implementation of the new CMC care coordination benefit, including the progress made and challenges that remain in coordinating care for dual eligibles. Results are summarized from 94 key informant interviews with health system stakeholders.
Many people with disabilities who get paid help with daily activities also need help with health maintenance tasks, such as ostomy care, ventilator management, bowel and bladder care, tube feeding, insulin injections, and management of other medications. In many states, laws prohibit paid workers without nursing or other medical licenses from performing such tasks. In others, nurses are permitted to delegate such tasks to these workers. In some instances, such workers can perform health maintenance tasks under the direction of the consumer, without nurse delegation or supervision.
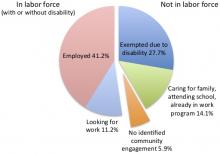
In January 2018, the Centers for Medicare and Medicaid Services (CMS) issued guidance that would allow states to use 1115 Waivers to add “work and community engagement” requirements for working-age Medicaid beneficiaries. This report examines the extent to which disability affects working-age Medicaid beneficiaries, and identifies the subset of beneficiaries with disabilities and work-limiting health conditions who would likely be exempt from proposed Medicaid work requirements or would benefit from modified requirements.
