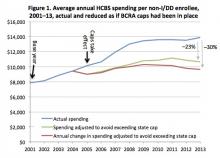
The Better Care Reconciliation Act (BCRA) proposes to cap Federal Medicaid reimbursements to the states on a per-enrollee basis, effectively limiting growth to a rate at first only modestly exceeding the rate of inflation in healthcare costs and then falling below inflation. If the BCRA were to be enacted, it is reasonable to assume that most states would limit home and community-based services (HCBS) spending to the per-enrollee cap amount; otherwise, any excess comes entirely out of the state budget.
Reports & Publications
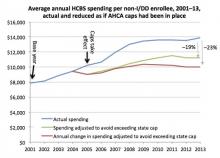
AN UPDATED VERSION OF THIS REPORT, BASED ON THE SENATE'S DRAFT BETTER CARE RECONCILIATION ACT, IS NOW AVAILABLE.

Abstract: This study examines health services appraisal (HSA) and unmet health-care needs for adults (age 50 and over) with physical disabilities in Medicaid managed care (MMC) versus Medicaid fee for service (FFS). Surveys from 309 individuals in MMC and 349 in FFS 2 years after MMC implementation included demographics, MMC processes, HSA, and unmet health-care needs.
As part of the University of California’s three-year evaluation of the Cal MediConnect (CMC) program, this research brief examines the efforts of CMC health plans to identify and transition members from long-term care institutions to home and community-based settings. Findings describe the progress many CMC plans have made in accelerating transitions out of institutional care, including successful strategies and challenges encountered in the process, as well as the barriers that still remain.
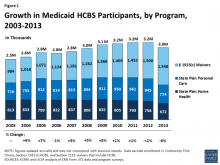
This report summarizes the key national trends to emerge from the latest (2013) participant and expenditure data for the three main Medicaid HCBS programs: (1) the mandatory home health services state plan benefit, (2) the optional personal care services state plan benefit, and (3) optional § 1915 (c) HCBS waivers. It also briefly discusses the provision of Medicaid HCBS through § 1115 demonstration waivers and highlights findings from a 2015 survey of Medicaid HCBS participant eligibility, enrollment, and provider reimbursement policies, including those related to the U.S.