In Iowa, training requirements for personal care aides are minimal compared to training requirements for home health aides and nursing assistants. Since 2006, Iowa’s long-term care leaders have been striving to create a competency-based training and certification system that spans all direct care workers and ensures high-quality care across populations and settings. While state lawmakers haven’t enacted training requirements for personal care aides, Iowa’s long-term care leaders have achieved promising results.
Reports & Publications

Arizona is among just 19 states that have enacted uniform training requirements for personal care aides (PCAs) across all Medicaid long-term care programs. The process by which the state adopted these training standards spanned from 2004 to 2012. During that time, home care leaders deliberated extensively over how to achieve a system that ensured a baseline level of competency among PCAs, while balancing the priorities of workers, consumers, providers, and the state. What was the need for PCA training standards in Arizona? How did home care leaders address that need?
The second in a series of research briefs by the UCSF Community Living Policy Center and the UC Berkeley Health Research for Action Center, this latest research brief examines the efforts of CMC health plans to coordinate behavioral health services for their beneficiaries. The brief describes the progress CMC plans have made toward better coordination of behavioral health services, including new integrated models of care, successful strategies, and ongoing challenges.
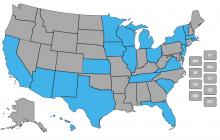
We reviewed managed long-term services and supports (LTSS) contracts for nine states in order to understand the extent to which they promote physical and programmatic accessibility for enrollees with disabilities. Medicare/Medicaid duals demonstration contracts for Virginia, Illinois, Massachusetts, Michigan, New York, and South Carolina contain provisions that represent a ground shift in federal expectations and requirements for physical and programmatic accessibility of managed care organizations (MCOs) and the providers with whom they contract.

In 2014 California implemented a federal dual alignment demonstration that used a capitated managed healthcare model called Cal MediConnect (CMC) to integrate medical care and long-term services and supports (LTSS) for beneficiaries with both Medicare and Medicaid. These beneficiaries often have complex care needs, including multiple chronic conditions and disabilities. By 2016, 120,000 eligible beneficiaries were enrolled in the program.

