In 2014, California became one of 13 states to implement a financial and administrative alignment demonstration called the Coordinated Care Initiative (CCI). In California, existing Medicare and Medi-Cal (California’s Medicaid program) managed care health plans in seven counties created new products called “Cal MediConnect” (CMC). Researchers from the University of California conducted an evaluation of the impact of the CMC program on beneficiaries and health systems.
Reports & Publications
Researchers from the University of California have conducted an evaluation of the impact of the Cal MediConnect (CMC) program on beneficiaries and health systems. One goal of CMC was to decrease expenditures through incentives to redirect care away from institutional settings and toward more home- and community-based services (HCBS). This research brief includes results from an in-depth examination of the efforts of CMC health plans to administer HCBS through their new managed long-term services and supports programs.
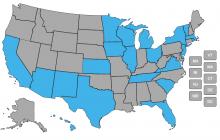
Over the course of the last decade, the United States has seen a significant increase in the use of Managed Long Term Services and Supports (MLTSS) within the Medicaid program. In order to ensure that MLTSS systems deliver high-quality services to people with disabilities and do not involve inadequate or overly medicalized service provision, states adopt certain requirements within their procurement for and contracting with MCOs.
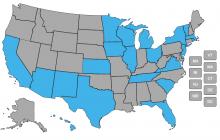
In Medicaid or Medicaid/Medicare managed long-term services and supports (LTSS) programs, states pay managed care organizations (MCOs) a per-member-per-month fee, or "capitation payment," which they structure to achieve policy goals. States often provide financial incentives that encourage MCOs to provide members with sufficient home and community-based services (HCBS) so that institutional placement can be avoided, and to work to transition institutionalized members back into the community. These incentives can help states “rebalance” their LTSS systems, meaning that they increase the pr

For years, training standards for personal care aides in Washington posed several challenges that affected consumers and workers alike. In 2012, advocates responded by successfully passing a ballot initiative that created a new training system for these aides—expanding learning objectives, increasing training hours, and introducing certification requirements. In just a few years, Washington raised the bar nationwide for training and certification. This report is part of a three-part series focusing on states that have led the way in developing personal care aide training standards.
