Although state use of Medicaid home- and community-based services (HCBS) to provide long-term services and supports to older adults and individuals with physical disabilities continues to increase, progress is uneven across states. We used generalized linear models to examine state factors associated with increased allocation of Medicaid dollars to HCBS for the period 2000 to 2011. We observed enhanced growth in states that began the period with limited investment in HCBS, as reflected in significant year trends among these states.
Reports & Publications

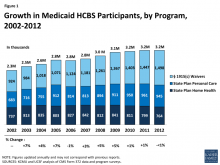
As states continue to implement various aspects of the Affordable Care Act (ACA), developing and expanding home and community-based alternatives to institutional care remains a priority for many state Medicaid programs.
Over the past several years, the State of Illinois has been implementing and planning several programs to move Medicaid and Medicare recipients into systems of care coordination. The original, mandatory Medicaid managed care program (MMC) in Illinois is known as the Integrated Care Program (ICP) and began on May 1, 2011 with the goal of improving the quality of care and services that the Medicaid population receives, along with saving the State money on Medicaid expenditures (estimated at $200 million over the first 5 years).

Researchers, policy experts, and advocates participating in an invitational conference discussed research needed to address pressing policy issues in long-term services and supports (LTSS). Future research on need for LTSS should focus on projections of need, geographic variations, equity, and unmet needs of consumers and caregivers. Research on access to home- and community-based services (HCBS) should address progress in rebalancing LTSS in favor of HCBS, cost-containment strategies, the shift to managed LTSS, and the performance of managed care organizations.
Provides a state-by-state look at trends in wages for personal care aides, a key job title within the direct-care workforce. Prepared as a resource guide on wages for advocates and policymakers concerned with the direct-care workforce, the chart book underscores the problem of poverty-level wages for PCAs, a factor that contributes to workforce instability for this high-demand workforce. The report finds that the national median wage for PCAs was $9.67 an hour in 2013 -- which is five percent lower than the median inflation-adjusted wage in 2003.
